How big a threat is Covid in North Carolina right now?
As of March 14, 99.9% of people in NC posed no threat of passing along COVID-19 to anyone, and about 47 of 50 (94.4%) of adult North Carolinians are estimated to have some level of immunity, either through at least partial vaccination or previous infection.
Active cases, which are the ones who can spread the virus, represent just over 0.3% of NC’s population. (note: active cases are lab confirmed cases of COVID-19 minus recoveries and deaths).
Interestingly, however, is that for the week ending March 12, 42% of Covid cases were to people considered fully vaccinated.
Also of note, as of Feb. 28, 8.4% of fully vaccinated individuals had “breakthrough” cases of Covid, compared with 3.5% of those with previous lab-confirmed cases getting reinfected.
When you combine adults with natural immunity with those with vaccine induced immunity, 94.4% of all North Carolina adults have some level of immunity to Covid. Recall that Cooper’s standard of immunity was two-thirds (66.7%) of adult North Carolinians partially vaccinated. According to Cooper’s own metrics, North Carolina long, long ago achieved herd immunity.[1]
How serious of a threat is COVID to various age groups?
As you might suspect, COVID presents a somewhat significant risk to a small part of the population, and a very slight risk to the majority of the population.
The “case fatality ratio” (CFR) measures the percentage of confirmed cases that ended with a death (confirmed cases are those in which the patient was actively tested and the test confirmed their case). In North Carolina, the CFR for those under 65 is 0.26%, roughly one-fourth of one percent. For those under 50 the CFR drops to 0.084%, or just under one hundredth of one percent. For children the CFR falls to .0035%, or three and a half one-thousandths of one percent, a survival rate of 99.9965%.[3]
But confirmed cases represents just a fraction of everybody who actually had COVID. Many more people no doubt had COVID, but for various reasons never tested for it, often times experiencing mild symptoms. According to the Centers for Disease Control and Prevention, only about 1 in 4.2 infections were reported. Which brings us to the “infection fatality ratio,” (IFR), which measures the percentage of infections that ended with a death. In other words, what share of those who ever had COVID died?
Even rounding down to 4.0 for the number of infections per confirmed cases, we find that for North Carolina, the IFR for those under 65 is .07%, or seven one-hundredths of one percent, and .021% for those under 50. North Carolina’s IFR for children is .0009%, for a survival rate of 99.9991%.
The CFR and IFR figures were calculated as of March 31, 2022.
While every death is tragic, these figures hardly represent the dystopian deadly disease portrayed by politicians and the media to justify never-ending draconian lockdowns and mandates.
It is important to note, however, that these death rates may be inflated as it has been widely reported that hospitals often reported deaths with COVID as deaths from COVID. So the deadly threat of COVID is likely even more remote than the DHHS data represents.
What about hospitalizations? Data on hospitalizations from COVID in North Carolina from NCDHHS for Oct. 1, 2020 to March 25, 2022 showed that roughly one in 6.5 hospitalizations (15.7%) were those aged 80 and up. Indeed, 57% of hospitalizations have been those aged 60 and up. Children aged 17 and below comprised just 1.98% of hospitalizations.[4]
Just 0.13% of children infected with Covid during that time required hospitalization. In other words, 99,870 of every 100,000 Covid infections in children did not require hospitalization.
And even among those that were hospitalized, a majority of those had pre-existing health issues. A study published in the Journal of the American Heart Association (JAHA) in late 2020 further revealed that nearly two-thirds (63.5%) of COVID hospitalizations were attributable to cardiometabolic conditions, including obesity, hypertension and diabetes. In short, those hospitalization would likely not have occurred if these conditions had not been present.[5]
Data on hospitalizations doesn’t tell us how long or how serious the hospital stay was, or if the patient entered the hospital with COVID or for another reason and then tested positive after admittance. Nevertheless, the data does reinforce the fact that hospitalizations for healthy people under 60 is quite rare.
Moreover, as even Dr. Anthony Fauci was recently forced to admit, when it comes to hospitalizations, especially children, “many of them are hospitalized with COVID as opposed to because of COVID.” This means that a not insignificant share of hospitalizations are people entering the hospital for non-Covid reasons and happen to test positive.
The bottom line: COVID never presented a significant risk to healthy people under age 60 or 65. Forcing one-size-fits-all quarantines, lockdowns, and mask mandates made little sense compared to a more focused approach directing most resources at protecting the sick and elderly.
Do mask mandates work?
To defend his mask mandates, Gov. Cooper’s office provided 22 studies, all published in 2020, containing what DHHS states is “overwhelming” “scientific evidence for the protective effect of face masks and respiratory virus infection in healthcare and community settings.”
Upon closer review, however, the studies presented by Cooper’s office did not justify the extreme use of mask mandates. The studies themselves at best were very uncertain over the effectiveness of masks at stopping the spread of COVID-19.[6]
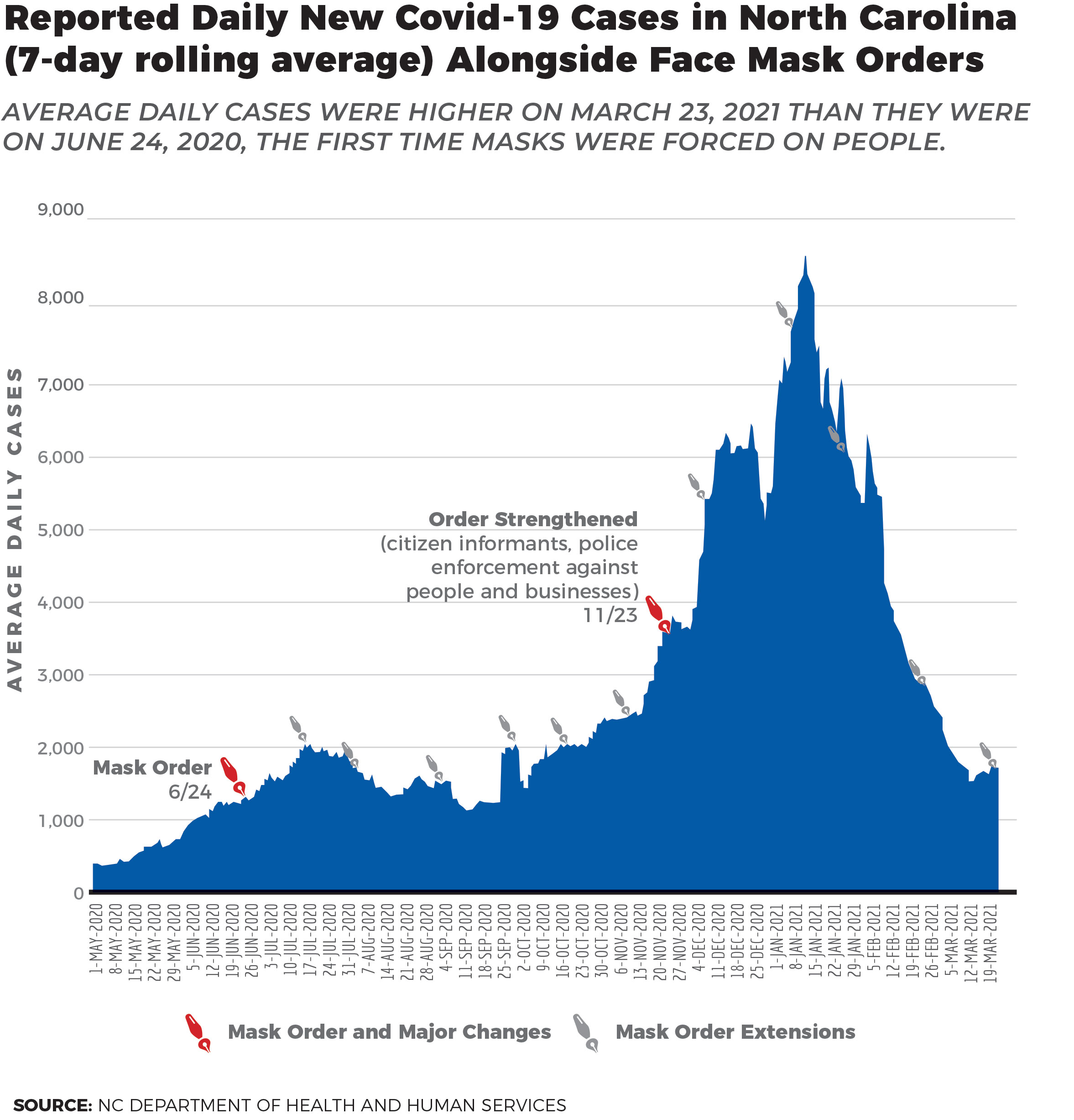
Indeed, the chart below shows that Cooper’s continued extension of mask mandates had no discernable impact slowing the spread of COVID.[7]
Masking healthy people doesn’t make sense. Indeed, it could do more harm than good. Last summer, the World Health Organization informed us “At the present time, the widespread use of masks by healthy people in the community setting is not yet supported by high quality or direct scientific evidence, and there are potential benefits and harms to consider.”
Healthy, asymptomatic people pose very little risk to others, but masks pose risks to the wearers. These risks, according to the WHO, include self-contamination, headaches, breathing difficulties, and facial lesions.[8]
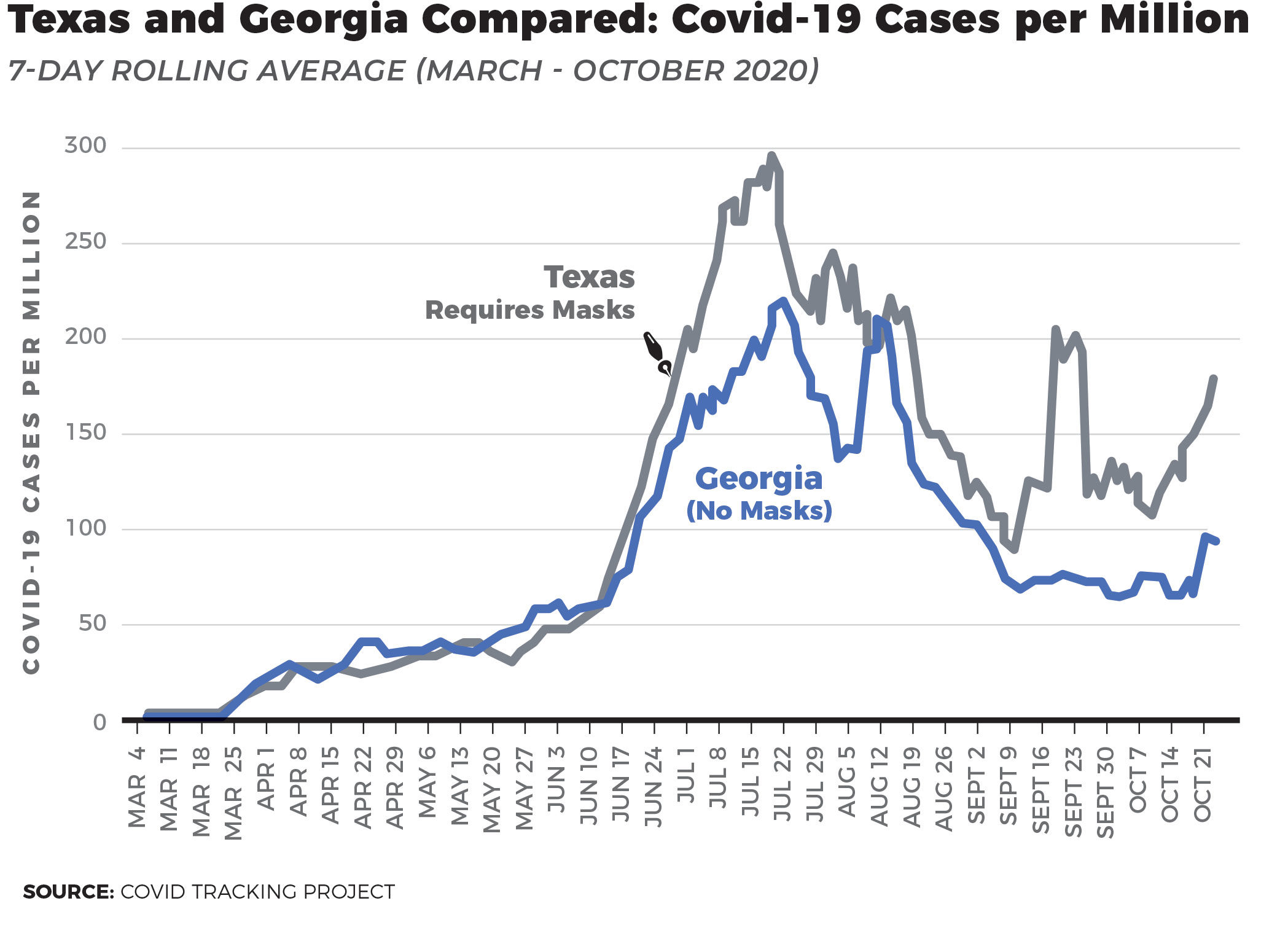
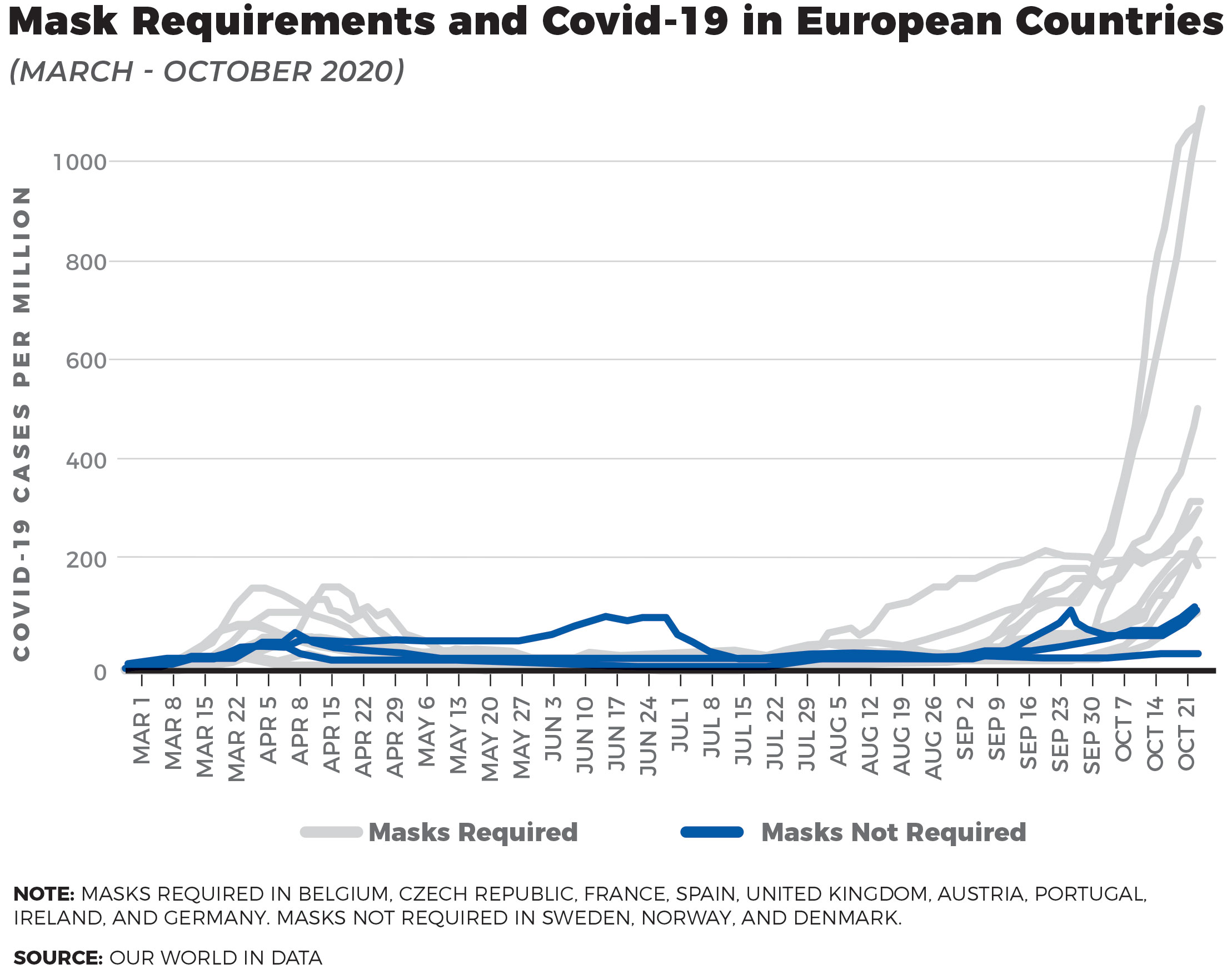
Some other graphs from last year comparing states and European nations show that mask mandates didn’t help slow the spread.
Was it safe to send children back to school?
Children have never been at serious threat from COVID. We’ve known this for a long time.
Perhaps the largest study tracking COVID transmission in schools last year was conducted in North Carolina. The findings were summarized in a Nature magazine article in July ’21.[9]
The study found that school-related transmissions were but a fraction of what one would expect given the infection rates of the surrounding areas. “Given the rate of transmission in the community, ‘we would have expected to see about 900 cases’ in the schools, says Daniel Benjamin, a pediatrician at Duke Clinical Research Institute in Durham, North Carolina, and co-lead author on the study. But when the researchers conducted contact tracing to identify school-related transmissions, they identified only 32 cases.”
Moreover, according to a July 2021 New Yorker magazine article[10], the “risk of severe disease or hospitalization is about the same” between COVID and the seasonal flu. Twice as many U.S. children died of pneumonia than died of COVID over the past year.
One CDC study[11] found the infection fatality rate for children aged 5-9 to be .001%, lower than that of the flu.
“All told, 600,000 Americans have lost their lives to COVID over the course of the pandemic; just 0.05 percent of those were under the age of 18, a population that represents more than 20 percent of the country’s population as a whole,” the article notes.
According to the article, “(I)n 2019, more than 2,000 American kids and teenagers died in car crashes,” nearly 6.5 times as many than died from COVID. Yet parents don’t hesitate to put their kids on school buses without seat belts driven by strangers with no hesitation to the risk.
And with more than 90% of North Carolina seniors now fully vaccinated,[12] there is little cause for concern that children may pass along the virus to their more vulnerable older relatives.
Should schoolchildren be forced to wear masks in school?
Given COVID’s extremely low risk to children, and the questionable – at best – efficacy of masks to prevent the spread of the virus, there seems to be little reason to mandate it. As of March 8, 2022, 105 of North Carolina’s 115 school districts have made masks fully optional. Indeed, Gov. Cooper recently changed his administrations guidelines to recommend that school districts lift their mask mandates. Yet many still insist that mandates in school should continue.
In a recent article in the Wall Street Journal co-written by Johns Hopkins doctor Marty Makaray and Tufts University chief of pediatric infectious disease H. Cody Meissner, the experts explored the question of “Do masks reduce Covid transmission in children?” Their answer? “Believe it or not, we could find only a single retrospective study on the question, and its results were inconclusive.”
By the end of Jan. 2022, even left-wing outlets including the New York Times and NPR are admitting that mandatory masking of school children likely does more harm than good.
Worse still, is the negative consequences and risks mask wearing imposes on children. Recent research from Florida[14] found that after just one day of use on a child’s face, masks become contaminated with pathogens and bacteria that threaten the child’s health. Upon six parents sending their children’s masks to a lab after one day of use, the results found “that five masks were contaminated with bacteria, parasites, and fungi, including three with dangerous pathogenic and pneumonia-causing bacteria.”
Indeed, top German scientists recently found that wearing masks for an extended period of time “could result in potentially hazardous chemicals and harmful microplastics being inhaled deep into human lungs.”[15]
As reported in an April article in Ecotextile News, the scientists determined that “mask wearers unwittingly run the risk of breathing in carcinogens, allergens and tiny synthetic microfibres by wearing both textile and nonwoven surgical masks for long periods of time.”
Given the virtual non-existent threat COVID poses to them, why would we want to force masks onto our children for extended periods of time?
Notes
[3] https://covid19.ncdhhs.gov/dashboard/data-behind-dashboards
[4] https://covid19.ncdhhs.gov/dashboard/data-behind-dashboards
[5] https://healthitanalytics.com/news/majority-of-covid-19-hospitalizations-due-to-4-chronic-diseases
[6] https://www.johnlocke.org/update/does-coopers-own-research-justify-his-extreme-orders-part-1/
https://www.johnlocke.org/update/does-coopers-own-research-justify-his-extreme-orders-part-2/
https://www.johnlocke.org/update/does-coopers-own-research-justify-his-extreme-orders-part-3/
[10] https://nymag.com/intelligencer/2021/07/the-kids-were-safe-from-covid-the-whole-time.html
[12] https://covid19.ncdhhs.gov/dashboard/data-behind-dashboards
[13] https://www.newsobserver.com/news/coronavirus/article254103783.html