For now. HB 283,The Telehealth Fairness Act, would have required insurance companies to pay medical providers for any health service provided via telemedicine that is otherwise covered during an in-office visit. Telemedicine has proven to be a cost-effective method to deliver care, and 32 other states already have similar telemedicine parity laws on the books. The game changer with North Carolina’s bill, however, is that all telemedicine services under this mandate would be reimbursed equal to the same treatment performed in a physical office setting.
This bill, if passed, would have added to North Carolina’s 57 health benefit mandates. Benefit mandates are requirements in which insurance companies must cover or offer expanded health care services that benefit particular patients and providers. They increase the cost of health insurance premiums, and stifle the ability for insurers to offer health plans that tailor to individuals’ needs.
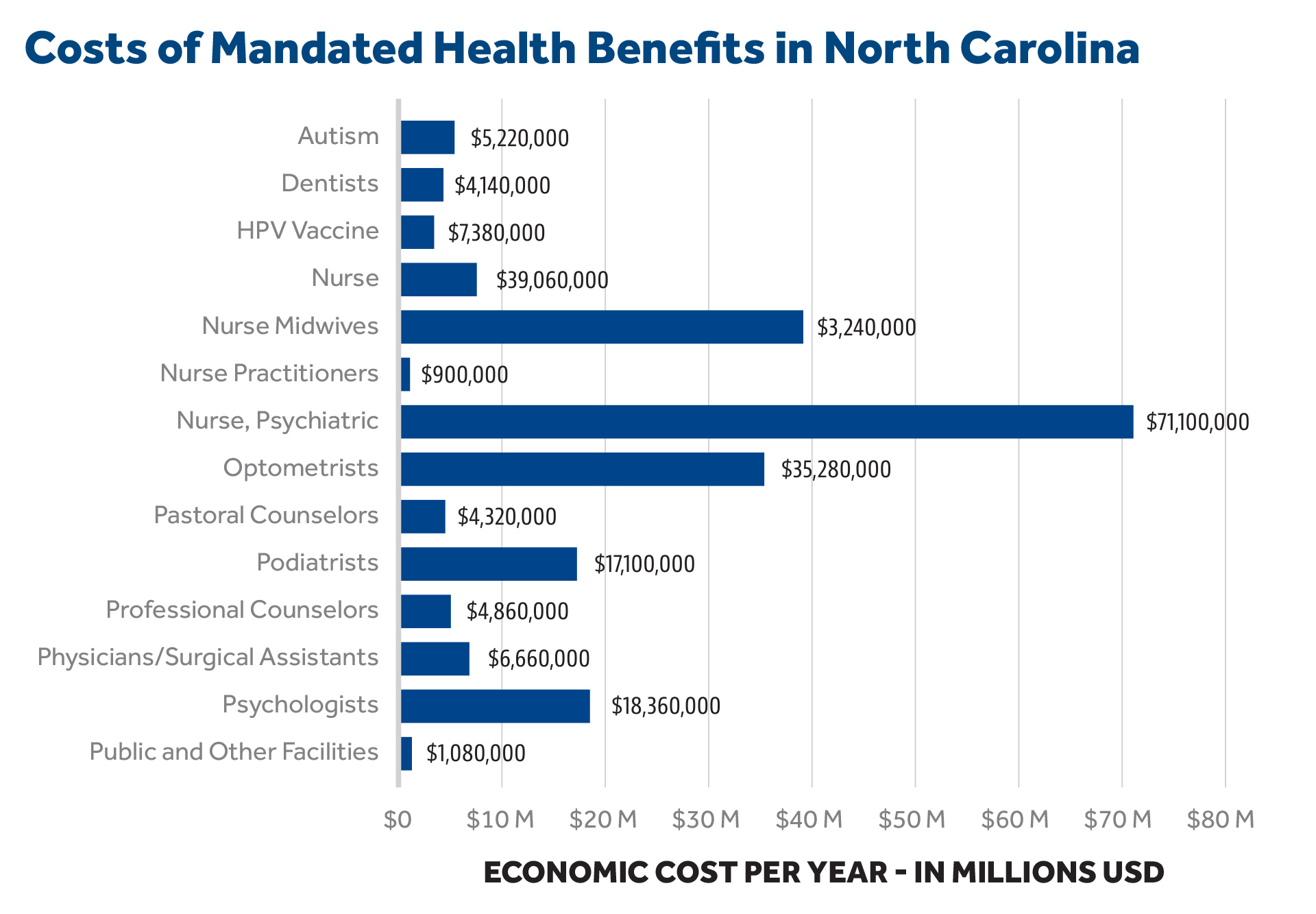
The following charts provided by the North Carolina Coalition for Fiscal Health estimate that they cost North Carolina policyholders in the individual and small-group insurance markets over $218 million per year:
Further movement on the telemedicine health mandate bill has been delayed. The House Health Committee has directed the Department of Health and Human Services (DHHS) to oversee a study on telemedicine policy before any mandates become effective.
Improving access to health care is important, but coverage mandates aren’t the solution to access decent treatment. The market has been working to extend important services to patients without paternalistic advances. In regards to telemedicine, insurers such as Blue Cross and Blue Shield of North Carolina have decided on their own to offer plans that cover telemedicine for psychiatric care, psychotherapy, health behavior assessments, diabetic counseling, and more. Since 2015, UnitedHealthcare members can choose from multiple service providers to engage in virtual office visits for under $50 – an innovative way to alleviate primary care physician shortages and medically underserved areas of the state. Direct primary care (DPC) physicians who don’t accept insurance provide telehealth as a value-added benefit that is included in their patients’ monthly membership fees.
For more information, click here to keep reading.