- An analysis of CDC estimates and DHHS deaths data for North Carolina finds that North Carolina has been witnessing more excess deaths than COVID deaths
- These worrisome findings seem to confirm research and experts’ warnings about the potential net deadlier effects of government lockdowns and severe personal and business restrictions, such as from Gov. Roy Cooper’s executive orders
- This analysis is limited by DHHS’s tardy data reporting to the CDC, even as Cooper continued to issue even stricter orders against people and businesses
In Part 1 of this series, I discussed research findings and experts warning that government lockdowns and severe personal and business restrictions may be deadlier than the virus they’re meant to protect people from, including in North Carolina. I discussed an earlier research brief finding that North Carolina was suffering excess deaths without even counting COVID-19 deaths.
I showed that delinquent reporting of deaths data to the Centers for Disease Control and Prevention (CDC) by the NC Department of Health and Human Services (DHHS) meant the CDC’s Excess Deaths metric could not be used as an early warning. Those data are much too late to alert Gov. Roy Cooper and his administration that his lockdowns and severe personal and business restrictions are creating more harm than good.
How late? Cooper’s DHHS is three and a half months behind the rest of the nation. As of March 3, the rest of the nation has submitted data through February 13 (incomplete after about mid-January). DHHS has submitted data only through October 31 (incomplete after September 19). Not only does the Cooper administration not have completed death data even into Fall 2020, but the greater implication is that Cooper has been basically flying blind issuing stricter orders and restrictions. They included a curfew, early business closures, tighter limits against people getting together, and a stricter face mask mandate.
Part 2 of this series will use estimates from the CDC and DHHS’s limited data reporting to see whether and to what extent North Carolina has been witnessing excess deaths outside of deaths attributed to COVID-19.
Charting non-COVID excess deaths in NC since the original lockdown
From what data we have from the CDC and the Cooper administration’s reporting, however, we can see that not only have there been excess deaths in North Carolina from COVID-19, but also that there have been excess deaths in NC from something other than COVID-19. I ask again: Are Cooper’s lockdown and restrictions exacerbating excess deaths in North Carolina?
Below is a graph based on the CDC’s average expected deaths per week for NC since March 27, 2020 (when Cooper’s original, “thirty days … to slow the spread” lockdown was announced) through Sept. 19, 2020, when DHHS’s reported deaths data were mostly complete. The baseline is the average expected deaths (a number from the CDC that varies per week, ranging from 1,723 the week ending Aug. 1 to 1,931 the week ending Mar. 28), the orange line is the upper bound confidence interval above which excess deaths are said to occur, the blue part of the bars represents the deaths for each week minus deaths attributed to COVID (i.e., the above-average non-COVID deaths), and the gray part of the bars represents the COVID deaths for each week as reported by DHHS. (See Part 3 for further explanation of the graph and its data.)
Here is how to interpret this graph: If the blue part of a week’s bar is visible at all, it means the week had above-average deaths that can’t be blamed on COVID. If any part of the bar exceeds the orange line, it means the week had excess deaths. If the blue part of a bar exceeds the orange line, it means the week had excess deaths that can’t be blamed on COVID — i.e., that something other than COVID is also responsible for excess deaths in NC that week.
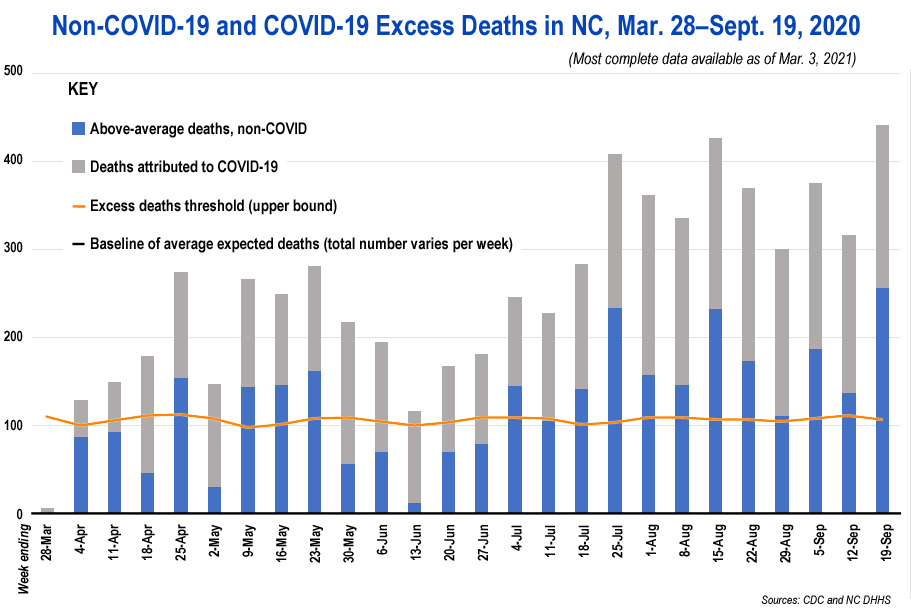
As you can see, since the very first week of the Cooper shutdown, North Carolina has seen at least above-average deaths without counting COVID deaths. Worse, North Carolina has suffered non-COVID excess death events in April, May, and steadily since July. This excess death event on top of the COVID-19 excess death event looked to be getting worse by the week ending Sept. 19 (the last week for which we have good data).
This analysis makes an even more disturbing finding. For the weeks ending April 25, May 9–23, July 4, and July 18 on through the data limitation of Sept. 19, North Carolina was witnessing more excess deaths than COVID deaths, underscoring how great was the increase in non-COVID deaths.
These findings suggest the effects of Cooper’s lockdown and severe personal and business restrictions have indeed been deadly, confirming the warnings from scientists, physicians, economists, mental health experts, and others over the past year.
This other, non-COVID death event — how bad did it get, or how bad has it gotten in the ensuing months? We can’t know, because the Cooper administration’s data reporting is so incomplete and far behind. Would Cooper have kept his orders all in place if he knew back in the fall about these non-COVID deaths? Would he have tightened them as he did? We can’t know that either.
But lives have been in the balance as DHHS dithered and Cooper kept tightening orders. They still are.
Part 3 of this series will provide the data from the CDC and DHHS used to make the graph, use a sample week to demonstrate how to apply the data, and include an explanation of the different categories, all in the hopes of bringing more clarity to what is a very real threat still facing North Carolinians.


