Yesterday’s front page of the News & Observer features the North Carolina Hospital Association, a free-market lobbyist, and legislators battling over pending legislation that could potentially terminate the state’s highly bureaucratic Certificate of Need (CON) law. Senator Tom Apodaca favors full-blown repeal, as this would open up competition in the health care market and enable patients to enjoy lower health care costs. Medical providers including hospital systems would no longer have to ask the state and their competitors permission to build new facilities, expand existing ones, or add or update major medical equipment.
Basic economics tells us that restricting supply increases costs for consumers — which is exactly what this current law does.
Hospitals, however, counter that health care is an exception to economics 101 because the price-controlling government has had such a strong presence since Medicaid and Medicare passed in 1965. For the most part, health care is not a free-market, so they believe that the way to ease the burden of this over regulated environment is to maintain or add more regulation in the form of CON.
Non-profit hospitals fear that if CON reform yields more multi-specialty physician-led ambulatory surgery centers (ASCs), these facilities will not only take away volume from their most lucrative outpatient service lines, but also go on a cherry picking spree for private coverage patients. Should this happen, community health systems will be left to care for revenue-losing patients — those who are either uninsured or on Medicaid.
The cherry picking argument is used frequently. Yesterday’s article paraphrases Cody Hand, chief lobbyist for the North Carolina Hospital Association:
Removing certificate-of-need laws will not create a fair and free healthcare marketplace. One example: Unlike same-day surgical centers, hospitals are required by federal law to treat and stabilize all who come to their emergency rooms, regardless of whether they have insurance or the ability to pay.
In an op-ed published in last month’s News & Observer, the CEO of Halifax Regional Medical Center writes:
Government payers like Medicare and Medicaid are responsible for two-thirds of all hospital patients but don’t compensate hospitals for the actual cost of care. Hospital payment rates set by government are nonnegotiable, often less than 60 percent of actual costs.
Nonhospital providers have the option of turning away patients who are uninsured and underinsured, such as those who rely on Medicaid. Those who would like to see CON weakened or repealed aren’t seeking to provide emergency care or to stay open 24 hours a day to respond to disasters. Under current regulations, they are not required to provide care for the uninsured patient.
And in yet another news article, Pardee’s CEO says:
As you look at ambulatory surgery centers and look at the payer mix of free-standing surgery centers owned by physicians and hospitals, the payer mix is much different in the free-standing center than it is in the hospital. Someone shows up in our ER, whether they’re off the street or whether they’re Bill Gates, we have to treat them. Can’t turn them away. We cast a broad safety net for this county. We just think ‘leveling the playing field’ is another way of saying cherry picking.
If there’s no margin, there’s no mission. I get that. But the current deal community hospitals have with the feds is that in order to not pay property tax, sales tax, or income tax, they are required to care for any patient who walks through their doors, regardless of their ability to pay.
For now, legislators should pay no heed to the patient cherry picking claim. Based on data from 2014 facility license renewal applications, the charts below illustrate that the payer mix is pretty comparable between existing multi-specialty physician-led ASCs and surgery centers partially or wholly owned by hospitals. It’s ironic that hospitals persistently use this argument when overall the surgery centers they are affiliated with take more commercial patients than for-profit surgery centers.
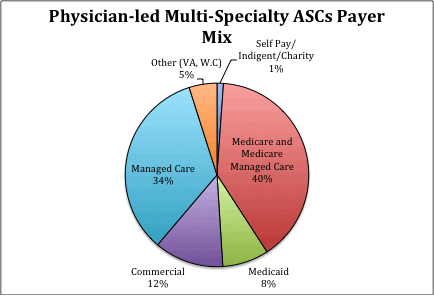
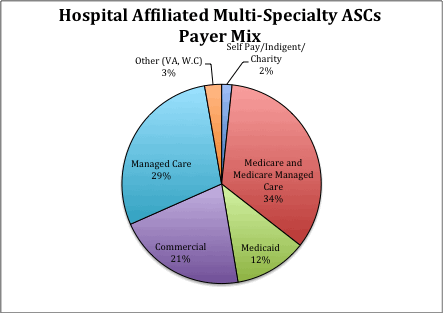
Click here for the Health Care Update archive.
You can unsubscribe to this and all future e-mails from the John Locke Foundation by clicking the "Manage Subscriptions" button at the top of this newsletter.


