When it comes to reforming our nation’s health care system, both sides of the political spectrum point to the "triple aim" — reduce health care costs, improve quality and access, and increase individuals’ overall health.
Now that Obamacare has added millions more to public and private health insurance roles, demand for health services will most likely increase — but by how much? Some can now for the first time access private coverage with a generous subsidy. Others now grudgingly pay substantially higher premiums coupled with an increase in deductibles and out of pocket costs.
Whether or not future data reveals a pent-up demand for health care, increasing the supply of health services and price transparency are just two ways to place downward pressure on costs.
My previous newsletters on North Carolina’s Certificate of Need (CON) program pertain to the health care supply/demand issue. CON laws intend to restrain health care costs by preventing duplicative services and proliferation of low-volume facilities. However, limiting the provision of health care upholds artificially high prices and stifles competition. As the program stands, if medical providers have plans to build or expand an existing health care facility, offer new services, or update or purchase major medical equipment, they will most likely have to apply for a "certificate of need" from the Division of Health Services Regulation, an arm of North Carolina’s Department of Health and Human Services (DHHS).
In the 2013 legislative session, state leaders and some physicians were on board to relax our state’s CON central planning process. Although initiatives failed to gain momentum, two bills (HB 83 and HB 177) sought to amend CON regulations by expediting the bureaucratic review process for certain proposed projects, eliminating diagnostic centers from needing a certificate of need, and increasing monetary thresholds that trigger review prior to construction or the purchase of replacement medical equipment.
Another incremental change would allow providers to add more operating rooms to existing outpatient surgical facilities without CON approval and enable providers to submit an unlimited number of applications to establish new specialized outpatient surgical settings. There are some "gaps," however, in this component. Providers interested in opening up an independently owned outpatient setting (where services cost less than hospital affiliated outpatient centers) would still be subject to the lengthy CON approval process and would face legal battles by surrounding competitors.
Beyond just surgeries, costs differ for other services between hospitals and independent health care facilities. The Wall Street Journal provides a good visual below:

Meanwhile, increasing price transparency plays a huge role in reducing health care costs. Imagine if more surgery centers or hospitals posted prices for procedures. Below is a snapshot of The Surgery Center of Oklahoma’s menu of surgeries and their respective average charges:

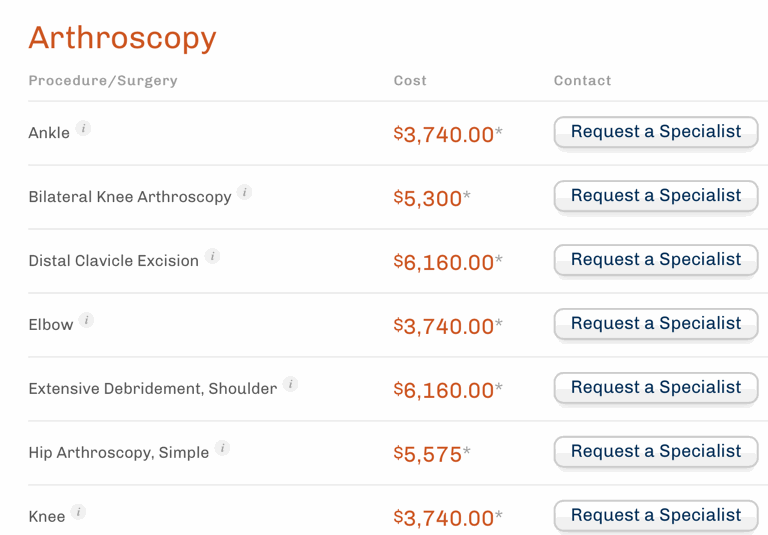
Lastly, insurers could welcome reference pricing, where a defined amount of money can be offered to a patient for surgery — enough to cover the cost of a procedure in some facilities, or the patient could negotiate with other facilitates that charge higher prices. Reference pricing has proven to be successful for the California Public Employees’ Retirement System.
Whatever the mechanism, reduced regulation and increased transparency will help move the health care system closer to realizing the triple aim.
Click here for the Health Care Update archive.
You can unsubscribe to this and all future e-mails from the John Locke Foundation by clicking the "Manage Subscriptions" button at the top of this newsletter.


