My colleagues Don van der Vaart and Jon Sanders have argued in a series of reports on the “fog of COVID-19 data” that coronavirus statistics are being miscalculated, misconstrued, and misused. An examination of hospital reporting, testing anomalies, and demographic variations corroborate their findings.
Hospitals
Hospitals have varied in their reporting of data. It seems different hospitals report each day with the percent of hospitals ranging from the mid-70s to the low 90s, so increases and decreases are sometimes based on reporting. On July 18, the state began reporting hospitalizations and the percentage of hospitals that provided data on the most recent day in each of the eight regional preparedness coalitions. The state now also reports new suspected and confirmed COVID-19 hospital admissions in each region.
Despite the improvements, unreported beds are still combined with beds that are reported as unstaffed. It is not clear how many COVID-19 hospitalizations were initially reserved for coronavirus patients or another condition like pregnancy. Hospitals survive by filling beds, so capacity utilization doesn’t answer questions; it only raises more. Hospitalizations as a share of cases are down, which fits with a number of hypotheses: 1) an increase in the number of cases and spread to younger people and those without comorbidities, 2) weakening disease through mutation, or 3) more time in the sun for people which means more vitamin D, heat and humidity as enemies of the coronavirus.
The number of people admitted to hospitals with a suspected or confirmed COVID-19 case fell from an average 543 the week of July 6-12 to an average 481 the week of July 13-19. Of those, suspected cases were 79% in the earlier week and 76% in the later week. The combined number of newly admitted patients was 43% of total hospitalizations. COVID-19 patients in ICU beds have increased from a low of 270 to a high of 340 in recent weeks. The only regions that have had relatively consistent growth in hospitalizations over the past month are the Triad and Charlotte.
Testing
Hospitalizations should be a function of cases and testing. In March, the state had few tests and restricted who could be tested to only those with severe cases with comorbidities, but the new hospital data do not go back that far. Despite expanded availability of testing over time, tests were still restricted by doctors into July, four months after voluntary suspensions of business and gatherings.
Antibody tests being done by Wake Forest University and others are not included in the NC Department of Health and Human Services (DHHS) reporting. We know the race, ethnicity, and languages of contact tracers but no indication of how many are needed or how well they have been able to trace contacts. Recoveries have been reported only in a pdf document with no history.
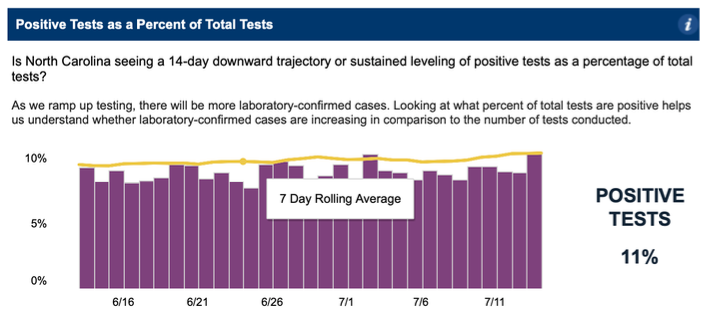
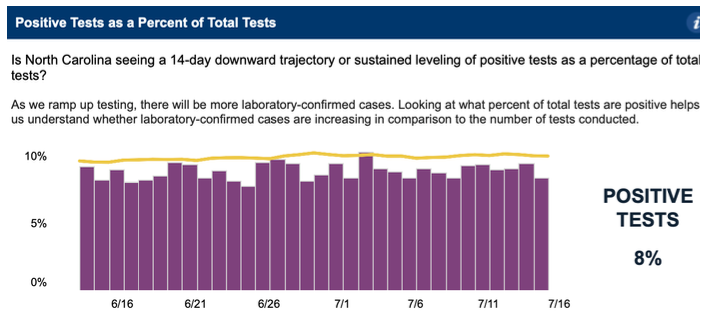
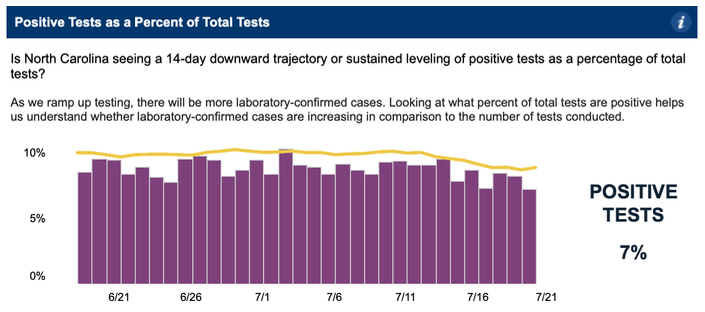
Percent positive is based on a subset of tests from labs that report both positives and negatives electronically. DHHS has not made the raw numbers available, so we can’t know how big the subset is. Moreover, the 7-day average is somehow consistently above the daily rates for the prior seven days. The rounded percent positive each day from July 3 through July 12 was either 8% or 9%, before reaching 11% on July 13, a number that was later revised to 10%. But the rolling average across the entire period was 10% to 11%. Clearly, there is something wrong with the calculation, as can be seen in the three graphs below.
July 14
July 15
July 20
Demographics
Nationwide, COVID-19 seems to affect African Americans and Hispanics more than other races and ethnicities, though in different ways. As of July 28, Hispanics make up 42% of cases, but just 11% of deaths. In contrast, African Americans are 24% of cases and 32% of deaths. There are reasons to worry about racial disparities, but it is not clear that systemic racism is to blame unless you expand that phrase to be practically meaningless.
Because the state does not provide race/ethnicity data in conjunction with age, it is impossible to know from the dashboard whether older African Americans in nursing homes made up most of the cases or what other factors may be involved. Indeed, age is the most widely recognized risk factor for death from COVID-19. Fully 69% of cases, as of July 28, are among people under 50, 88% are under 65, and 94% are under 75, but 57% of deaths are from the 5% of people with COVID-19 aged 75 and older, and 95% of deaths are among people 50 and older. Still, 29% of cases (34,000) have no reported race and 35% (41,000) have no reported ethnicity. There have been at least 769 deaths in nursing homes and another 153 in residential care facilities. Numbers could be higher because 257 deaths have missing information.
Conclusion
Charles Piller in Science Magazine wrote states’ refusal “to share highly specific information for their COVID-19 cases, which some scientists warn is hampering efforts to identify targeted measures that could stem the spread of SARS-CoV-2 without full-scale lockdowns.” If we are going to triumph over this virus, then we need greater data transparency and stronger accountability for those precluding it.